
Dear Members (a note from Deb Hickey):
My favorite musical group growing up was the English rock band, Duran Duran. My walls were adorned with posters and pictures of John Taylor, Andy Taylor, Roger Taylor, Nick Rhodes, and Simon Le Bon (interestingly, none of the Taylors were related). My goal in life was to one day marry the bass player, John (still is, but I don’t tell my husband).
Some 40 years later, “Rio,” released in 1982, is still one of my favorite songs and I’ll often blast it on my car stereo and sing at the top of my lungs. The band is still touring and coming to Boston (I’m about 20 minutes southwest) in September. I keep going back and forth as to whether the $300+ tickets are in my budget.
Why in the world am I writing about my favorite childhood band? Last month, I heard that Andy Taylor, guitarist and founding member, was diagnosed with stage 4 prostate cancer at the young age of 56. In an article in People magazine, Mr. Taylor is quoted as saying, “As harsh as it is, it’s a death sentence. So, you sort of walk out of the hospital in a stunned silence, because you could never be prepared for ... you’ve got to start from the fact that it’s a slow burn, so it’s not going to take you quickly.”
Last week I spent about two hours trying to find a phone number or an email address – any means for getting in touch with Mr. Taylor. I actually connected with a woman who used to work directly with the band, but she wasn’t in contact with them anymore.
At this late stage in his disease, Mr. Taylor likely isn’t a candidate for protons, but I was desperate to inform him about theranostics – an extraordinary new technology for treating certain aggressive and metastatic cancers, including prostate, that we’ve written about in several BOB Tales newsletters. Perhaps if I could have reached him, I could have changed his outlook. Alas, I was unsuccessful in all my attempts.
I guess it’s true what they say – cancer doesn’t discriminate. Even my favorite, life-long celebrities aren’t immune.
So, I’ll use this story as a reminder to you, our members, to educate your brothers, sons, nephews, and grandsons about early PSA testing. Tell them that, because they have cancer in the family, they should start testing at an early age to get a baseline PSA.
I know some of you spread the word about testing as well as proton therapy and other treatment modalities by buying and sharing my father’s book. Others forward this newsletter to dozens of others, every month. By doing this, you could be saving a life – or many lives.
-------------------------
This month’s BOB Tales is stuffed with important information on prostate cancer testing and imaging, healthful eating to protect against the disease, and more. We first tell you about a new study which has uncovered the mechanism that enables cancer to metastasize. Scientists believe we may now have a way to slow down or even stop cancer cells from spreading. There’s also a new study on prostate cancer imaging using an experimental “F-18” PSMA radiotracer which is exceptionally effective in detecting recurrent prostate cancer. And a newly enhanced urine test may lead to better detection of high-grade disease. Our Flashback article focuses on several examples of successive rises in PSA where no recurrences were found. I’m also happy to introduce BOB member Ed Dodson in our Giving Back section. Ed says his proton therapy is “the closest thing to a miracle” he’s witnessed since the birth of his children. And he shares his father’s important life lessons and how they relate to his treatment and the life he’s living now. Can plant-based diets really lower your risk of prostate cancer? Find out what researchers have to say after reviewing 32 studies which evaluated possible links between vegetarian diets and prostate cancer risk. And there’s much more!
As always, we love to get feedback on the newsletter and welcome any suggestions you have on how to improve the value of the BOB Tales to our members. Just send an email to [email protected].
Deb Hickey
P.S. If any of our 10,000 members has an idea for connecting with Andy Taylor (or knows him personally – hey, you never know), please let us know! :)
To print the BOB Tales newsletter or view the newsletter with a larger font size, click here for the PDF file.
.jpg)
In This Issue:
- New Study Uncovers Potential Target for Stopping 90 Percent of Cancer Deaths
- PET/CT with Tracer May Improve Prostate Cancer Imaging
- Urine Test Effectively Detects Aggressive Prostate Cancer
- Three Successive Rises in PSA – And No Cancer Recurrence
- Can Plant-based Diets Lower Your Risk of Prostate Cancer?
New Study Uncovers Potential Target for Stopping 90 Percent of Cancer Deaths
Metastasis (meh-TAS-tuh-sis): The spreading of cancer cells from the primary tumor into surrounding body tissues and organs/the leading cause of death in cancer patients
An international team of researchers has uncovered the mechanism that enables cancer to spread throughout the body. This groundbreaking discovery may provide a way to stop deadly metastases responsible for 90 percent of cancer deaths.
According to the study, cancerous cells move faster and become more aggressive in thicker fluids, a change that happens when lymph drainage is disrupted by a primary tumor.
“This is really the first time the viscosity of the extracellular fluid has been looked at in detail,” said John D. Lewis, professor and Bird Dogs Chair in Translational Oncology at the University of Alberta’s Faculty of Medicine & Dentistry.
Lewis’ lab was invited to join the project team, led by researchers at Johns Hopkins University, because of its “expertise in imaging human cancer cells in real-time motion using the placenta-like chorioallantoic membrane from fertilized chicken eggs.”
“I would say we’re the world leaders in this type of imaging,” said Lewis. “Our contribution to the work was to very precisely show that cancer cells change their gene expression when they encounter increased viscosity in the surrounding fluid and become more aggressive. And even when you bring the viscosity back down, these cells stay more aggressive.”
Through trials on mice, the researchers learned that when this signaling pathway is disturbed, it changes cancer cells’ ability to metastasize.
“Now that we know that fluid viscosity signals cancer cells to move in a specific way, we can potentially use drugs to basically short-circuit that signaling pathway and encourage cancer cells to slow down, or maybe even to stop,” said Lewis.
Lewis believes it may take up to 15 years to develop and test these new drugs.
PET/CT with Tracer May Improve Prostate Cancer Imaging
PSMA is a protein found primarily on the surface of prostate cells. It’s present at a low level in normal prostate cells, but the amount is markedly higher in prostate cancer cells.
PSMA PET imaging can detect microscopic prostate cancer cells that would otherwise have been missed by traditional imaging methods. And, since PSMA-PET can also precisely detect cancer that’s spread beyond the prostate, it’s shown that biochemical recurrence
of the disease doesn’t always spread in a systematic way – it sometimes shows up in unexpected areas of the body. This revelation is changing how imaging is conducted, thereby widening the field of view to include more parts of the body.
According to a new study, PET/CT imaging with an experimental F-18 prostate specific membrane antigen (PSMA) radiotracer is exceptionally effective in detecting recurrent prostate cancer – so much so, it could have significant implications in decision-making treatment plans for the majority of prostate cancer patients.
Gallium-68 PSMA-11 – a highly sensitive drug that’s proven to be highly effective in detecting prostate cancer throughout the body – received FDA approval in 2020. As researchers continued to explore alternatives, they found that tracers labeled with F-18 could expand availability to satellite clinics because the isotope has a longer half-life than Gallium-68.
Researchers also found the F-18 PSMA-1007 PET/CT to have superior sensitivity and the highest inter-reader agreement compared with standard and advanced prostate cancer imaging modalities.
► BOB Comment: We wrote about Gallium-68 PSMA imaging in our February 2021 issue of BOB Tales. At the time, we believed it should have become the new standard-of-care for initial prostate cancer staging as well as evaluation of patients with recurrent cancer because it’s so precise. But we’ve heard the F-18 PSMA may be even better.
Urine Test Effectively Detects Aggressive Prostate Cancer
Prostate cancer is multifocal – it generally occurs in multiple parts of the prostate – and heterogeneous – even within the same tumor from the same patient, tumor cells might be subtly or even dramatically different. Researchers sought to determine what’s really responsible for how cancer will behave in individual patients.
The typical methodology for detecting cancer after an elevated PSA reading or abnormal prostate exam is to do a biopsy. Though the blind biopsy is still the standard-of-care, there have been improvements to the procedure. For example, an MRI-guided prostate biopsy can identify “hot spots” or regions of interest to target, thereby improving the detection of the disease. But even with the use of MRI, 10 to 15 percent of high-grade prostate cancers are missed, according to Simpa Salami, MD, MPH, Assistant Professor, Department of Urology, University of Michigan.
Researchers under the direction of Dr. Salami aimed to build upon their previous urine-based test, developed back in 2013, called the Michigan Prostate Score, more recently rebranded as the “My Prostate Score.” The test was developed to detect aggressive prostate cancer in urine. In looking to improve the test with the help of evolving technology, researchers determined they could identify molecular changes that may be different from patient to patient. They found the molecular profile in any given tissue may be different within the same region of cancer, or within different areas of the prostate. The researchers are confident that with this new test, they can capture what’s going on in the entire prostate, which may lead to better detection of high-grade disease.
We’ve been producing BOB Tales newsletters for more than 20 years. During this time there have been articles that many new members haven’t seen, and some older members may have forgotten. So, we periodically re-run articles from past newsletters. The following is from May 2007.
Three Successive Rises in PSA – And No Cancer Recurrence
Picture this: You finished your proton treatment and your PSA drops from the mid-5’s to 1.8. This is good news. Six months later it bumps slightly to 2.0. Not a big worry – bumps are common. In another six months it’s 2.8. And two months after that it rises to 5.0. Now you’re concerned. Your urologist concludes that your cancer has returned and suggests you start hormonal therapy. What do you do?
One of our members had this experience and he suggested to his urologist that he repeat the PSA test. The doctor disagreed and reiterated his recommendation to begin hormonal therapy.
Not comfortable with his doctor’s advice, he sought a second opinion from an oncologist who ordered another PSA test. The result was 1.8. One month later it was 1.7. That was two and a half years ago. Today his PSA is 0.3 and holding steady. It was a false alarm.
Here is some more interesting information. A member recently sent us an article titled, “Clinical Correlates to PSA Spikes and Positive Repeat Biopsies after Prostate Brachytherapy.”
The article reports on a study conducted on several men who had brachytherapy (radioactive seeds) for their prostate cancer. Eight of the men in the study saw their PSA initially decline, and then turn around. Each experienced three to five successive increases in PSA, all within 30 months of treatment. Biopsies on every one of these men showed cancer in the prostate.
But here’s the interesting part: In all eight cases, no action was taken; PSA turned around, began to decline, and settled down at nadirs of less than 1.0.
The Study’s Conclusion
Transient PSA rises can occur even in the presence of a persistently positive biopsy, and patients and physicians should not feel compelled to rush ahead with salvage therapy. On the basis of the patient data reported here, it appears that a spike up to 10 ng/ml is still consistent with cancer eradication.
This is significant, as we believe it can also apply to other forms of radiation therapy.
What conclusions can we draw from this?
- PSA bumps – even multiple PSA bumps – don’t necessarily mean your treatment has failed. So don’t panic if you see one, two or even three rises. But you shouldn’t ignore them either.
- Always seek a second or third professional medical opinion before embarking on a new course of treatment.
- According to Buckminster Fuller: “There are no straight lines in the universe.” Don’t try to predict your post-treatment PSA pattern. It will be different for everyone.

“Just Make a Difference”
 When BOB member Ed Dodson had an elevated PSA reading in 2011 at the age of 69, he was surprised. “Nobody in my family has had prostate cancer that I’m aware of,” said Ed. “For many years, since my family doctor started checking my PSA as a precaution, my measurements always ran anywhere from 0.1 to 0.3.” But at one of his annual appointments, Ed’s PSA came back at 4.0. “My doctor was concerned, so she referred me to a urologist,” said Ed.
When BOB member Ed Dodson had an elevated PSA reading in 2011 at the age of 69, he was surprised. “Nobody in my family has had prostate cancer that I’m aware of,” said Ed. “For many years, since my family doctor started checking my PSA as a precaution, my measurements always ran anywhere from 0.1 to 0.3.” But at one of his annual appointments, Ed’s PSA came back at 4.0. “My doctor was concerned, so she referred me to a urologist,” said Ed.
Surgery – Unacceptable!
After a biopsy, Ed was shocked to learn he had Gleason 9 prostate cancer. “My urologist immediately recommended I have a prostatectomy,” said Ed. “But that wasn’t acceptable for several reasons – namely, the side effects associated with surgery. On top of that, I had three friends who had surgery for their prostate cancer – two died and the other had terrible pain and months of recovery.”
Fortunately, Ed had a few friends from church in his hometown of Salem, OR that had been treated for prostate cancer and they were doing great. “They all had this treatment called ‘proton therapy’ at Loma Linda University Cancer Center in California,” said Ed. “And they all had good results.”
When Ed asked for his urologist’s opinion on proton therapy, he advised against it. “He considered it an experimental approach to a serious situation,” said Ed.
“I went ahead and called LLUCC anyway,” said Ed. “After they ordered a full body scan and learned my cancer hadn’t escaped the prostate gland, I was accepted into treatment.”
An Enjoyable Experience
Ed described his experience of treatment as pleasant. “I definitely didn’t feel like I was being treated for cancer,” he said. “With the exception of the balloon insertion – which was a little embarrassing and uncomfortable – I enjoyed that 15 minutes of daily treatment. The technicians were so friendly and caring. In fact, the whole hospital is that way! I loved every single one of the Loma Linda staff members who were involved in my healing. They brought a Christian attitude to everything they did.”
Ed also received hormonal treatment due to the aggressiveness of his disease. “I was initially concerned about the side effects of hormones,” Ed said. “But it wasn’t a problem at all. I had a tiny bit of breast enlargement, but I can live with that.”
Ed also enjoyed the camaraderie among patients at LLUCC. He attended every Wednesday night meeting and several dinners out during his stay.
Most Successful Prostate Cancer Patient
Ed just celebrated his 82nd birthday. “I clean my gutters, do all my own yard work, and get in about 10,000 steps a day during my walks,” he said. “My proton therapy is the closest thing to a miracle I’ve witnessed since the birth of my children. I’m truly blessed.”
Ed went back to the same urologist after his proton treatment ended. “At the end of two years, he released me,” said Ed. “But not before telling me I was his most successful prostate cancer patient! I suggested he consider recommending proton therapy to some of his patients.”
Ed’s Recommendations to Newly Diagnosed Men
“I’d recommend they find friends or acquaintances who’ve had prostate cancer,” Ed said. “Find out what treatments they had and ask them about their experiences and outcomes. I’d then give them this phone number – 1-800-PROTONS.”
Ed said if he hadn’t had conversations with his friends about their health, he may never have found proton therapy. “It’s so important to talk to others,” he said.
Giving Back
“I donate to several health and education-related organizations,” said Ed. “I was raised by a father who had an extremely tremendous sense of core values, and I adopted most of them.” Ed’s father taught him to give more than you receive. He also told him to leave everything better than he found it. “And you don’t need to do that at great cost,” Ed said. “I volunteer to mow cemataries and church lawns and I give back monetarily when I can,” Ed said. “If everyone practiced the two principals my father taught me, there’d be no need for police or jails.” Ed’s overall advice
is to “just make a difference.”

Giving Options
Online
From the pull-down menu, choose where you'd like to direct your gift — 1) Proton Research through the James M. Slater Chair, 2) Proton Research through the Robert J. Marckini Chair, or 3) choose "Other" and specify where you'd like your gift directed in the space provided.
By Check
- Make your check out to "LLUCC."
- Specify where you'd like to direct your gift in the memo line — 1) Slater Chair, 2) Marckini Chair, 3) Theranostics, or 4) write "Unrestricted" so LLUH can use it where it's needed most.
- Mail your check to: LLUH, Office of Philanthropy P.O. Box 2000, Loma Linda, CA 92354.
By Phone
- Call Regina Joseph at 909-558-5010.
Can Plant-based Diets Lower Your Risk of Prostate Cancer?
Researchers assessed 32 studies evaluating possible links between plant-based diets and lower prostate cancer risk. A third of the studies were observational – the research relied on pre-existing information contained in databases and health registries – and the rest were interventional – the participants were prostate cancer patients who had been followed over time.
In general, the studies leaned toward beneficial effects from consuming plant-based foods. Further, most of the observational studies found that those who ate mostly plant-based meals developed prostate cancer at lower rates than meat eaters. Sixty percent of the interventional studies reported that PSA levels increased more slowly in plant-based eaters compared to meat eaters.
The researchers concluded – based on the PSA findings, the delayed need for additional prostate cancer treatment, and overall improved health of plant-based eaters – that vegetarian diets help protect against prostate cancer. Further research, including large-scale clinical trials, are still needed to confirm the association.
Not enough data?
In a follow-up article, Dr. Stephen Freedland, a urologist and the director of the Center for Integrated Research in Cancer and Lifestyle at Cedars-Sinai Medical Center in Los Angeles, and his co-authors highlighted shortcomings in the existing data. For example, the interventional studies are small (fewer than 100 participants in each), with follow-ups lasting no longer than one year. They also argued that the observational evidence is hardly unanimous – some of the studies detected no association between prostate cancer risk and plant-based eating, while others generated mixed results.
More Questions
Another issue is lack of consensus on what constitutes a plant-based diet. Definitions range from complete vegan to semi-vegetarian where some meat consumption is allowed. “What we really need in this area are more rigorously designed, well-controlled randomized clinical trials,” Dr. Freedland said. “We need to sort out whether diet is really protective, or if vegetarians and vegans are simply more health-conscious in other ways. Are they exercising more? Do they have better access to health care? Do they live in places with better air quality? These are the questions we need to answer.”
Regardless, Dr. Freedland said the evidence associating plant-based diets and lower prostate cancer risk as intriguing and encouraging.
► BOB Comment: You know where we stand on this topic. We believe, no matter the amount of data or lingering questions about these 32 studies, the best lifestyle strategy for reducing overall cancer risk is to eat a healthful diet – which includes an abundance of fruit and vegetables – while reducing or eliminating meat consumption. We also recommend daily exercise!

Cauliflower Stir Fry
If you’re looking for creative ways to eat more vegetables, try this cauliflower stir fry recipe from the Prostate Cancer Foundation. The PCF touts the benefits of a plant-based diet citing a study authored by several researchers, which followed more than 47,000 health professionals over 28 years. Participants’ diets were categorized by scores based on the types of foods they ate – overall plant-based, healthful plant-based, and unhealthful plant-based – and how often they ate them. Eating a more plant-based diet overall was associated with lower risk of fatal prostate cancer.
Ingredients:
- 1 medium head cauliflower (2 pounds), chopped into small florets
- 1 red bell pepper, thinly sliced
- 1 orange bell pepper, thinly sliced
- 1 medium white onion, thinly sliced
- 3 green onions, thinly sliced
- 3 tbsp rice vinegar
- ¼ cup soy sauce (or tamari or coconut aminos)
- 1 tbsp light miso
- ½ tbsp gochujang (Korean chili paste -optional)
- 2 tbsp sugar (or maple syrup)
- 2 tbsp sesame oil (regular, not toasted)
- 1 tsp cornstarch (or arrowroot powder)
- 3 tbsp neutral oil for stir frying, divided
Directions:
- In a medium bowl, whisk together rice vinegar, soy sauce, miso, gochujang, sugar, sesame oil, and cornstarch.
- In large skillet, heat 2 tablespoons neutral oil over medium high heat. Add the cauliflower and a pinch of salt and cook, not stirring, for 3 to 4 minutes until charred. Flip the florets and continue cooking for 2 minutes.
- Add the bell peppers, white onion, a pinch of salt and the remaining 1 tablespoon oil and cook 4 to 6 minutes until tender.
- Turn off the heat. Pour in the sauce and add the green onions. Stir until the sauce coats everything and thickens. Serve immediately.

National Proton Conference
 The National Association for Proton Therapy (NAPT) is a non-profit organization founded to educate and increase public awareness about the clinical benefits of proton beam therapy. Founded in 1990, the NAPT advocates to ensure patient choice and access to affordable proton therapy and to encourage cooperative research and innovation to advance the appropriate and cost-effective use of proton therapy.
The National Association for Proton Therapy (NAPT) is a non-profit organization founded to educate and increase public awareness about the clinical benefits of proton beam therapy. Founded in 1990, the NAPT advocates to ensure patient choice and access to affordable proton therapy and to encourage cooperative research and innovation to advance the appropriate and cost-effective use of proton therapy.
Each Spring, NAPT holds an annual conference, the National Proton Conference (NPC), that brings together leaders in the field of particle therapy with a robust agenda focused on emerging clinical research, operational efficiencies, insurance authorizations, and in recent years a partnership with PTCOG-NA to present a special session.
Deb Hickey plans to attend NPC 2023 – “Elevating Access, Research, and Innovation in the Field of Particle Therapy” – in Salt Lake City, UT, May 6-9.

 You Can Beat Prostate Cancer: And You Don’t Need Surgery to Do It – Second Edition
You Can Beat Prostate Cancer: And You Don’t Need Surgery to Do It – Second Edition
195 Amazon Reviews
As of this writing, there are 195 reviews on Amazon, almost all five-star, and the book is in the No. 2 position on a general search for “prostate cancer” in the books category.
Following is a recent review by a doctor from Rhode Island:

A Five Star Review – A Foundation and Understanding of Prostate Cancer
This book should literally be required reading for anyone diagnosed with prostate cancer, and who is starting to review the options of treatment being presented.
Mr. Marckini has been given a gift of a passion for what he went through deciding on treatment for himself. He has also been given a talent for natural writing skills. By the end of the book, the reader feels he has made a friendship with a wonderful advisor and feels able to negotiate the journey one is about to take, deciding on the prostate cancer treatment of choice for himself.
Mr. Marckini not only makes you feel like you have found a friend but also a well-educated and thoughtful professional to help you through this very emotional, challenging, and important decision and time.
This book is a must-read for those diagnosed with prostate cancer. I would further recommend that men of 50 years and older read this book, in preparation for what appears to be an important discussion that many aging men may need to come to grips with. This prostate cancer diagnosis is a very common occurrence for a huge male population. As a doctor myself, I have found that an informed patient will feel more confident in his decision making. In my practice, I always had the philosophy that, “The way you feel is the way you heal.” This book will make the reader feel very well.

The Personal Side
Last month we continued with our series of excerpts from Chapter 9 of Bob’s latest book, switching from the technical stuff to the personal side of Bob’s experience of treatment, looking back on the events of 22 years ago. In previous BOB Tales we reported on Bob & Pauline’s arrival in Southern California; events leading up to the start of treatment; his relief on learning that his treatment was truly painless and uneventful; his realization that he made the right treatment decision; his daily routine; his proton technology education process; and the importance of proper nutrition while in treatment.
This month we’ll cover the importance of maintaining emotional fitness and the role Wednesday night meetings played in that process.
Emotional Fitness
Psychological or emotional health has been shown to enhance physical health and strengthen the immune system, which helps prevent disease and hasten the healing process.
As mentioned earlier, radiation works by damaging the cancer cells’ DNA, preventing the cells from reproducing. Healthy cells damaged by radiation typically repair themselves and reproduce, while the damaged cancer cells eventually die off. Clearly both processes – healthy cell repair and cancer cell death – are enhanced by a healthy emotional state and a positive mental attitude.
Scientific studies have shown that emotional and psychological factors can positively or negatively impact the immune system’s ability to fend-off diseases of all kinds, including cancer.
As mentioned earlier, the cancer center had established a social work department within radiation medicine as part of their effort to provide emotional/psychological support to patients while in treatment.
I’ve often been critical of the over-dependency of our culture on psychologists, psychiatrists and psychotherapists, and the small percentage of these practitioners who actually do their patients any good (I’ve seen some people harmed by their psychotherapists). However, I do believe there’s a place for competent psychologists, psychiatrists and social workers in our society.
The psychosocial programs at Loma Linda are amazingly effective. At the heart of these programs is the Wednesday night support-group meeting.
When I was doing my research and interviewing proton patients, the Wednesday night support-group meetings were frequently mentioned. I heard, “You must attend,” or, “Don’t miss a single one.” I put that advice aside, because of my belief that, “real men don’t do support groups.” I had visions of 50 people sitting in a circle, holding hands and singing Kumbaya. I couldn’t have been more wrong. My experience while there for my consult convinced me of that.
Since my treatments started on a Wednesday, I had the opportunity to attend my second Wednesday night support group meeting – the first for Pauline. We arrived just after 5:30, and at Pauline’s suggestion, planned to stay for an hour and then go out to dinner. We helped ourselves to some refreshments and entered the room. Once again, it was packed with about 90 people sitting around rectangular tables, and a few seated on folding chairs randomly placed in any available space. There were no empty chairs, and others were standing, so we decided to stand near the door so we could make our quiet exit.
The mood in the room was festive. People were laughing; and that didn’t make sense to Pauline, even though I had explained to her my experience of this meeting two weeks before.
Gerry Troy stood up and introduced himself. With a calm and sincere voice, he welcomed all of us, reminded us to help ourselves to some refreshments, and told us the location of the restrooms. The latter, I learned is important, as urinary urgency is a common temporary side effect of any radiation delivered to the pelvic region.
Gerry then made some announcements about group activities. Next, he read a poem and a couple of jokes, all sent to him by former patients, expressly for this meeting. These were well received, and we found ourselves laughing with the rest of the group.
He then asked if there were any alumni in the audience. Seven hands went up. He called on one of them – a gentleman about 60 years old from Arizona named Richard – who stood up and told his story. Richard began by announcing his pretreatment PSA and Gleason score. Then he talked about how his prostate cancer was discovered; his shock and disbelief; the meeting with his urologist who recommended surgery; his investigation of the alternatives; his discovery of proton treatment; the help he received from former proton patients; his physician’s unprofessional behavior when he heard Richard had chosen proton treatment (“Find yourself another urologist when you return!”); his wonderful experience of both treatment and his two-month stay in Southern California. He then reported his most recent PSA, 0.9, which drew spontaneous applause from the audience.
This process was repeated six more times. The PSAs, Gleason scores, and home states varied, but the stories were very similar: They all looked beyond their urologist’s first recommendation; did their homework; investigated their options; got help from former proton patients; chose proton therapy; and had a wonderful experience.
To be continued …

Was Bob's book helpful to you?
If Bob’s book was helpful to you and you’d like to help others find it on Amazon, please write a review. Book reviews help boost the book’s visibility within Amazon’s search results for users looking for information on prostate cancer treatments and/or proton therapy.
Proceeds from book sales are used to help fund our efforts and to support proton therapy research.


Last Month’s Brain Teaser
You have black socks, blue socks, green socks, and gray socks in your drawer. There are twice as many black socks as blue socks. There are three times as many black socks as green socks. There are twice as many gray socks as green socks. In the dark, how many socks do you need to pull out of the drawer to be sure you’ll get a pair of matching socks?
Answer: Note, we didn’t specify any particular color, just a matching pair. You need to take five socks to be sure of a pair. If you pull out only four, then you could have black, blue, green and gray. The proportions of socks in the drawer are irrelevant.
Winner: We had a record last month for the most guesses ever submitted – there were hundreds! Either the teaser was too easy, or our members are getting smarter!
The lucky winner for February is BOB member Bob Bielenberg formerly of Nevada City, CA. Bob was treated with proton therapy for his prostate cancer at Loma Linda University Cancer Center in 2008. “All the staff at Loma Linda made the process almost fun,” said Bob. While in treatment, he attended weekly Wednesday night patient meetings, Tuesday potluck dinners, meals out at local restaurants, and had “great conversations with the staff, other patients, and their partners.”
It’s been 15 years since Bob’s proton treatment ended and he’s feeling well and has a low and steady PSA. Bob has moved to Palm Springs, CA where he works part-time in the construction industry and keeps active by riding his bicycle and swimming.
“I am so grateful for my health and especially grateful to have found Loma Linda for my proton treatment,” said Bob.
Congratulations, Bob! Your signed copy of Bob Marckini’s book is on the way!

New Brain Teaser
Tom has three, Dick has three, and Harry has three. How many do they all have together?
Hint: The answer is not nine.
Send your brain teaser answer to [email protected] for a chance to win a signed copy of Bob Marckini’s NEW second edition book, You Can Beat Prostate Cancer.

Poor Norman
I asked Old Maud how she lost her husband, Norman. She told me her sad story …
“Well, my sweet Norman was in the hospital and needed a blood transfusion immediately, but his blood type was not on record. So, the doctors asked me if I knew what it was, as they urgently needed to know, in order to save my Norman’s life! But I’ve never known his blood type, so the only thing I could do was sit with him and say goodbye … I’ll never forget how compassionate and supportive my Norman was. Even as he was fading away, he kept whispering to me, ‘Be positive; be positive!’ That was my Norman … He was always thinking of others.”

Memorable Quotations
“The difference between stupidity and genius is that genius has its limits.” – Albert Einstein
“It would be nice to spend billions on schools and roads, but right now that money is desperately needed for political ads.” – Andy Borowitz
“At every party there are two kinds of people – those who want to go home and those who don’t. The trouble is, they’re usually married to each other.” – Ann Landers
“The surest sign that intelligent life exists elsewhere in the universe is that it’s never tried to contact us.” – Bill Watterson
“As a child my family’s menu consisted of two choices: take it or leave it.” – Buddy Hackett
“My favorite machine at the gym is the vending machine.” – Caroline Rhea
“Never, under any circumstances, take a sleeping pill and a laxative on the same night.”
– Dave Barry
“We’re here on earth to do good unto others. What the others are here for, I have no idea.” – W.H. Auden


Longest Lasting Cars, SUVs, EVs
According to the organization, iSeeCars, the average lifespan of a typical car from the 1970s was 100,000 miles. Today, they report the lifespan of a modern car to be 200,000 miles.
Are you looking to purchase the last car you’ll ever need? iSeeCars studied over two million used cars that were on the road between January and October 2022. Last month, they ranked them based on the top one percent of cars within each model obtained. Cars included in the study are limited to those with at least 10 years of production, which limited the EV options.
Following are the top cars in each category:
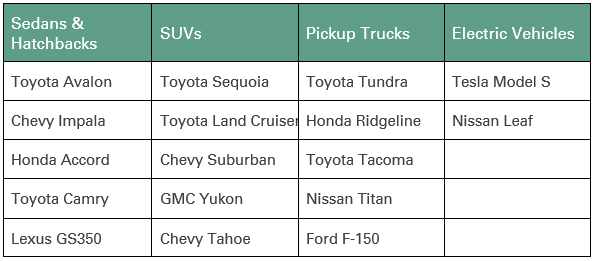
Click here for more details and the complete list of vehicles in each category.

Car Keys and Home Security
Put your car keys beside your bed at night. If you hear a strange noise outside or think someone is trying to get into your house, press the panic button for your car. The alarm will go off and continue to sound until you turn it off or the car battery dies.
Your car alarm is a security system you probably already have, and it requires no installation!
If an alarm sounds, odds are a burglar won’t stick around. After a few seconds, all the neighbors will be looking out their windows to see what’s going on. A criminal won’t want that!
Also remember to carry your keys while walking to your car in a parking lot. The panic button can work the same way in that situation.
This is something that should be shared with everyone. Maybe it could prevent a serious crime or even save a life.


The 1 Percent Age Group Source
This special group was born between 1930 and 1946 (16 years). In 2023, the age range is between 77 and 93. Are you, or do you know, someone in that age range? If so . . .
- You are the smallest group of children born since the early 1900s.
- You are the last generation, climbing out of the depression, who can remember the winds of war and the impact of a world at war which rattled the structure of our daily lives for years.
- You are the last to remember ration books for everything from gas to sugar to shoes to stoves.
- You saved tin foil and poured fat into tin cans.
- You saw cars up on blocks because tires weren’t available.
- You can remember milk being delivered to your house early in the morning and placed in the “milk box” on the porch.
- You are the last to see the gold stars in the front windows of grieving neighbors whose sons died in the war.
- You are the last generation who spent childhood without television. Instead, you imagined what you heard on the radio.
- With no TV until the 50’s, you spent your childhood playing outside.
- The lack of television in your early years meant you had little real understanding of what the world was like.
- On Saturday afternoons, the movies gave you newsreels sandwiched in between westerns and cartoons.
- Telephones were one to a house, often shared (party lines) and hung on the wall in the kitchen (no privacy).
- Typewriters were driven by pounding fingers, throwing the carriage, and changing the ink ribbon.
- INTERNET and GOOGLE were words that didn’t exist.
- Newspapers and magazines were written for adults and the news was broadcast on the radio in the evening. As you grew up, the country was exploding with growth.
- The government gave returning veterans the means to get an education and spurred colleges to grow. Loans fanned a housing boom.
- Pent up demand coupled with new installment payment plans opened many factories for work.
- New highways brought jobs and mobility.
- The radio network expanded from three stations to thousands.
- You weren’t neglected, but you weren’t today’s all-consuming family focus. They were glad you played by yourselves until the streetlights came on. They were busy discovering the post-war world.
- You entered a world of overflowing plenty and opportunity; a world where you were welcomed, enjoyed yourselves and felt secure in your future though depression poverty was deeply remembered.
- Polio was still a crippler.
- You came of age in the 50s and 60s. You are the last generation to experience an interlude when there were no threats to our homeland. The second world war was over, and the cold war, terrorism, global warming, and perpetual economic insecurity had yet to haunt life with unease.
- Only your generation can remember both a time of great war, and a time when our world was secure and full of bright promise and plenty. You grew up at the best possible time, a time when the world was getting better …
- You are “The Last Ones.” More than 99 percent of you are either retired or deceased, and you feel privileged to have “lived in the best of times!”
Low PSAs to all,
Bob Marckini and Deb Hickey
To print the BOB Tales newsletter or view the newsletter with a larger font size, click here for the PDF file.
NO MEDICAL ADVICE: Material appearing here represents opinions offered by non-medically-trained laypersons. Comments shown here should NEVER be interpreted as specific medical advice and must be used only as background information when consulting with a qualified medical professional.



